TCA Peel for Acne Scars: Everything You Need to Know
I know firsthand the struggle of finding an effective treatment for acne scars, especially one that won't break your bank account (like $1,000+ laser treatments!!).
Fortunately, chemical peels like trichloroacetic acid (TCA) are one of the best options to improve your scar appearance and promote a healthy-looking complexion. (1)
RELATED:
In this post, I'll explain what a TCA peel is (including TCA CROSS), the key benefits, the evidence from 27+ medical studies, potential side effects, and aftercare instructions.
But first, let's find out if a TCA peel is suitable for you.
RELATED ARTICLES:
Should You Get A TCA Peel For Acne Scars?

In my opinion, this depends on 3 factors:
1. What Type(s) of Acne Scars Do You Have?
If you have atrophic acne scars (such as rolling, boxcar, or ice pick scars), a TCA peel is an excellent way to remove the damaged scar tissue and stimulate collagen growth.
Over time, this allows healthy skin to grow back and fill in the "gaps" of these scars.
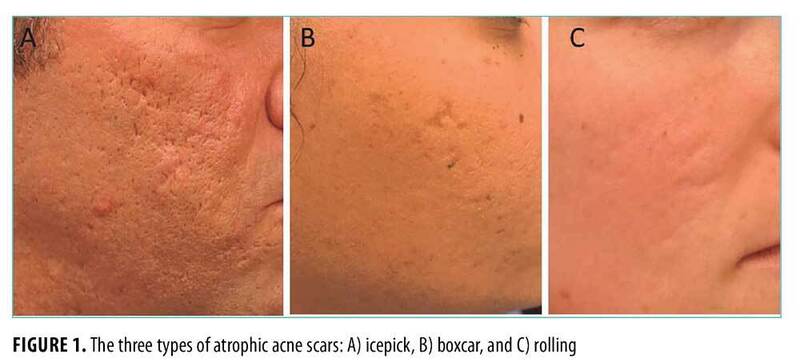
If, however, you have raised acne scars (such as hypertrophic scars and keloids), TCA might not be as effective since your main problem here is actually excess collagen.
A better option would be corticosteroid injections paired with silicone gels or sheets. (2)
RELATED:
2. What's Your Fitzpatrick Skin Type?
You may have heard of "Fitzpatrick skin type" at your dermatologist's office before.
Created by Dr. Thomas B. Fitzpatrick in 1975, the Fitzpatrick scale (1-6) reflects the level of melanin pigment in your skin (darker skin types have more melanin).
Here's an easy (and fun) way to identify your skin type from Game of Thrones:

If you have darker skin (III-VI), research shows that you're more likely to experience some side effects including hyperpigmentation, hypopigmentation, demarcation lines, and even further scarring (yes, unfortunately). (3, 4)
The most common complication is post-inflammatory hyperpigmentation (PIH), but you can reduce your risk of getting it by taking adequate precautions, such as:
- A pre-peel priming regimen of 2-4% hydroquinone (or another melanin inhibitor)
- A post-peel routine of avoiding sun exposure and religious sunscreen usage (4)
RELATED:
3. Do If You Have Any of These Contraindications?
Finally, it's a good idea to check if you have any of the following conditions:
- A history of post-inflammatory hyperpigmentation
- A history of keloids or poor wound healing
- A history of photosensitivity (sun sensitivity) or you work outdoors
- Recent usage of isotretinoin (Accutane, Retin-A, etc.)
- Recent cosmetic surgery
- Active herpes simplex virus (open cold sores)
- Sensitive skin or a history of atopic dermatitis
as these may increase your risk of potential complications. (3)
Speak to your dermatologist to understand the risks before proceeding with a TCA peel. For at-home peels, always start with a low concentration (10-15%) and work your way up.
What Is A TCA Peel?
Trichloroacetic Acid (TCA) is a popular, effective, and highly versatile chemical peel.
TCA was discovered as early as the 1880s (5) and was first documented by Monash (1945) as a potential treatment for acne scars, eczema, and other skin conditions. (6)
In the following decades, TCA has become widely used by dermatologists and patients for a variety of common skin problems, including:
- Acne Scars (especially ice pick scars, see TCA CROSS below)
- Hyperpigmentation (including melasma, dark spots, post-acne marks)
- Sun Damage (including age spots, scaly patches)
- Wrinkles, Fine Lines, and Sagging Skin
- General Skin Maintenance
The TCA peel is best described as a Swiss army knife.
It is highly versatile and can be adjusted by concentration and technique or combined with adjacent therapies to reach almost any part of the skin.
Consider the following chemical peel classification table by Gozali et al. (2015) (7):

Depending on the concentration and number of coats, TCA can be classified as a:
- Very Superficial Peel: 10% or lower (1 coat)
- Superficial Peel: 10-30% (generally 1 coat)
- Medium-depth Peel: 35-50%, with or without pretreatment like Jessner's Solution (Monheit, 1989), solid CO2 (Brody, 1989), or 70% Glycolic Acid (Coleman, 1994), that removes the epidermis to allow TCA to penetrate to the papillary (upper) dermis
In addition, as we'll see later in the medial literature, TCA is increasingly being combined with adjacent therapies (most notably, microneedling) to produce a deeper peel than what would normally be achieved by TCA alone.
What Is TCA CROSS?

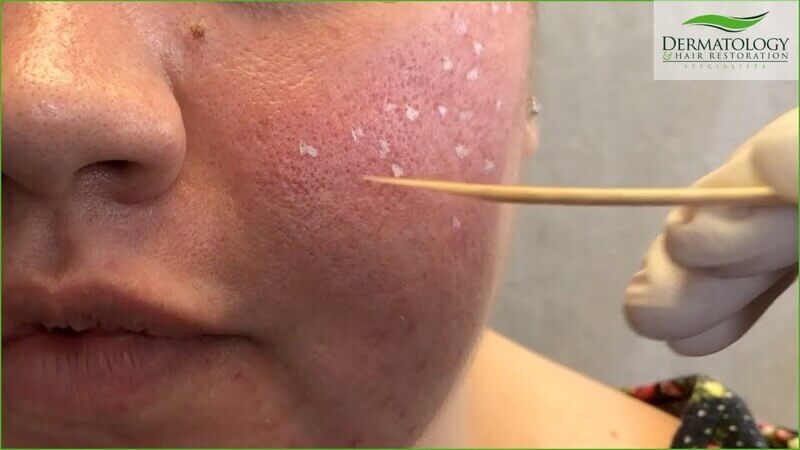
Chemical Reconstruction of Skin Scars (CROSS) is a popular and extremely effective technique that involves applying high concentration TCA (50-100%) directly to the base of atrophic acne scars using a wooden applicator (usually a toothpick). (8)
The CROSS technique was originally developed by South Korean doctors in 2002 and has been widely proven in the medical literature as an effective and inexpensive method of removing ice pick scars (narrow and deep puncture marks).
The advantage of TCA CROSS is that, unlike a full face peel, only the problematic areas are treated while the surrounding skin remains intact. This helps reduce the downtime as healthy skin cells can migrate to the new wound to speed up the recovery process. (9)
What Are The Benefits Of A TCA Peel?

There are many reasons to consider a TCA peel:
1. TCA Can Penetrate Deeper Than Superficial Peels
Unlike superficial peels like glycolic acid, TCA can penetrate beyond the epidermis into the papillary (upper) dermis to correct deeper acne scars (as well as wrinkles and fine lines) by stimulating new collagen growth and tissue regeneration in the dermis.
Consider this diagram of chemical peel penetration from Soleymani et al. (2018) (1)
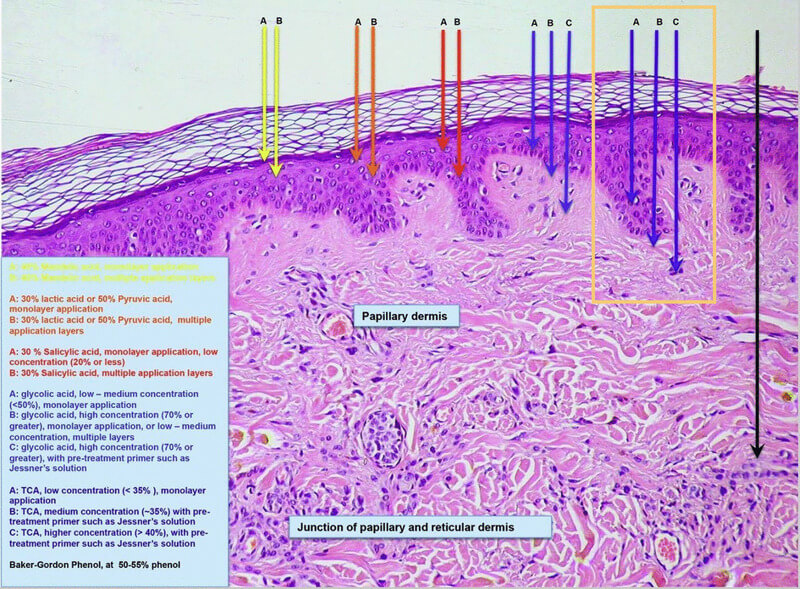
I know the text is probably too small to read, so here's a summary of what each line represents (from left to right):
- Yellow Lines: 40% Mandelic Acid (Superficial Peel)
- Orange Lines: 30% Lactic Acid or 50% Pyruvic Acid (Superficial Peel)
- Red Lines: 30% Salicylic Acid (Superficial Peel)
- Blue Lines: from left to right, <50% Glycolic Acid (Superficial Peel), >70% Glycolic Acid (Strong Superficial Peel), >70% Glycolic Acid with pretreatment primer (Medium Peel)
- Purple Lines (Highlighted): from left to right, <35% TCA (Superficial to Medium Peel, depending on concentration and technique), 35% TCA with pretreatment primer (Medium Peel), >40% TCA with pretreatment primer (Medium Peel)
- Black Line: Baker-Gordon 50-55% Phenol (Deep Peel)
As you can see, a 35% TCA peel (with or without pretreatment primer) is going to remove more layers of skin tissue (and address deeper skin problems) than any superficial peel.
The only peel that penetrates deeper is Baker-Gordon Phenol, which has fallen out of favor due to longer recovery times and a higher risk of complications. (1)
For beginners and at-home usage, however, I recommend starting with a 10-15% TCA peel which will provide a similar level of exfoliation as 50-70% glycolic acid. (7)
RELATED:
2. TCA CROSS Is Extremely Effective For Ice Pick Scars
Since the CROSS technique was developed in 2002, researchers have confirmed its effectiveness in multiple clinical trials around the world. (8, 10, 11, 12, 13, 14)
The pilot study by Lee et al. (2002) in South Korea showed that the targeted application of high concentration TCA (65% or 100%) led to good or excellent results in 27 of 33 patients in the 65% group (82%) and 30 of 32 patients in the 100% group (94%). (8)
Those are some very impressive numbers!
Further studies by Yug et al. (2006) and Fabbrocini et al. (2008) in the U.S. and Italy, respectively, showed that TCA CROSS produced long-term decreases in acne scar depth and increases in collagen fibers, as seen in skin biopsies and clinical examinations. (10, 11)
Fabbrocini also found that 50% TCA was effective for scar revision (instead of 90-100%).
Finally, 3 Indian studies conducted clinical trials with 12, 30, and 53 patients, respectively, using 70-100% TCA on atrophic acne scars (predominantly ice pick scars). Good or excellent results were recorded in 100%, 93%, and 66% of patients, respectively. (12, 13, 14)
Overall, TCA CROSS is an exceptional treatment for ice pick scars, and results in significant scar improvement and high patient satisfaction.
3. TCA Is More Affordable Than Other Scar Treatments
I know I definitely don't want to pay $1,000+ per session for laser treatments when there are more cost-effective options available (source: PlasticSurgery.org).
According to RealSelf, the average cost of a full face TCA peel is about $200 a session (source: RealSelf). The actual cost depends on your area, clinic, and practitioner.
The average cost of TCA CROSS is roughly $200 a session as well (source: LA Skin MD).
For comparison's sake, the average cost of microneedling is $100-$200 a session, microdermabrasion is $175 a session, and intense pulsed light (IPL) is $600 a session.
While microneedling can also stimulate collagen growth, it may not be as effective for deeper atrophic scars as the needles must penetrate into the papillary (upper) dermis in order to promote wound healing and collagen remodeling. (also, needles scare me!)
Microdermabrasion only provides surface-level exfoliation while IPL is about as expensive as most laser treatments (almost $2,000 after 3 sessions!).
Now, if you're comfortable with doing a TCA peel or CROSS at-home, you can save a lot on expensive dermatologist visits (because you're really paying for their time and expertise, not the actual material cost of the chemical peel).
For a 10-15% TCA peel for beginners, it costs under $30 for a 1.0 oz bottle which should last (conservatively) at least 10 treatments:
- I recommend the Perfect Image 15% TCA Skin Peel (I use this one myself)
For a 20-30% TCA peel for CROSS, it costs less than $60 for 1.0 oz (6 bottles of 0.17 oz) which could last a while depending on how many scars you're treating:
- I recommend the Platinum Skin Care 30% TCA Pro Peel
Is There Any Evidence From Medical Studies?

I wouldn't be called The Derm Detective if I didn't have any actual evidence.
That's why I've summarized 27 medical studies on TCA and TCA CROSS. You're welcome!
TCA Peel (20-35%) with or without Jessner's Solution
The following studies have found that TCA, with or without Jessner's solution, is a very effective treatment for atrophic acne scars, as shown by increased collagen formation and significant improvements in scar severity scores:
- Nelson et al. (1995): a single 35% TCA peel was performed on 3 male patients with actinic keratoses (pre-cancerous sun damage). Researchers compared biopsies taken before, 2 weeks, and 3 months after the procedure under electron microscope and found increased collagen type I and activated fibroblasts (special cells that produce skin tissue like the extracellular matrix and collagen). (15)
- Kang et al. (1996): a Korean study examined 23 patients with atrophic acne scars following multiple sessions of TCA peels (% not specified). Patients who had 6 or more sessions experienced good or excellent results in 13 of 15 cases (87%) while patients who had only 4 sessions did so in 4 of 7 cases (57%). (16)

- Al-Waiz et al. (2002): a combination Jessner's solution and 35% TCA peel was performed on 15 patients with both atrophic and ice pick scars. After 3 sessions, most patients experienced improvements in scar appearance as follows: moderate to significant (60%), minimal to mild (33%), and none (6.7%). (17)
- Carniol et al. (2005): researchers at Boston University examined 9 patients with atrophic acne scars (rolling, boxcar) following 4 monthly sessions of non-ablative laser treatment plus 2 additional bimonthly 30% TCA peels. The authors reported better results with the additional chemical peels compared to patients who only had the laser treatment. (18)
- Puri (2015): a study of 50 patients (2 groups of 25) compared Jessner's solution plus 20% TCA to 20% TCA alone. 6 sessions of chemical peel were performed at 3 week intervals. While there was no statistically significant difference, the JS+TCA peel produced marked improvement (i.e. 70% or more) in 60% of patients compared to only 28% in the TCA group. (19)
TCA CROSS (50-100%)
Next up, the following studies on TCA CROSS highlight the effectiveness of this technique for pitted and ice pick scars:
- Lee et al. (2002): the first study to use the CROSS technique for atrophic acne scars. 65 patients were treated with either 65% TCA or 100% TCA using toothpicks that were pressed hard into the scar to break down skin tissue and stimulate collagen growth. Good or excellent results were achieved in 27 of 33 patients in the 65% TCA group (82%) and 30 of 32 patients in the 100% TCA group (94%). In addition, all patients who received 5 or 6 sessions experienced good or excellent results which highlights the need for multiple visits. (8)
- Yug et al. (2006): a US study that replicated Lee et al. (2002) using 95% TCA on a group of only 3 patients. 6 sessions were performed at 6 week intervals. Clinical and histologic examination (under microscope) of punch biopsies taken at baseline and 1 year post-op showed a decrease in the depth of acne scars and an increase in collagen fibers and fragmentation of elastin fibers. (10)
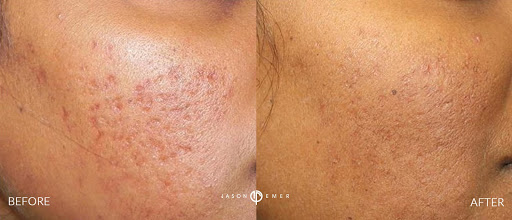
- Fabbrocini et al. (2008): an Italian study that used 50% TCA instead of 90-100% on a small group of 5 patients for acne and chickenpox scars. 3 sessions were performed at 4 week intervals. Clinical examination and digital photographic analysis showed improvements in both scar depth and appearance. (11)
- Bhardwaj et al. (2010): an Indian study that replicated Lee et al. (2002) using 100% TCA on 10 patients with predominantly ice pick scars. 4 sessions were performed at 2 week intervals. Excellent results (more than 70%) were seen in 8 of 10 patients evaluated and good results (50-70%) in the remaining 2 patients. (12)
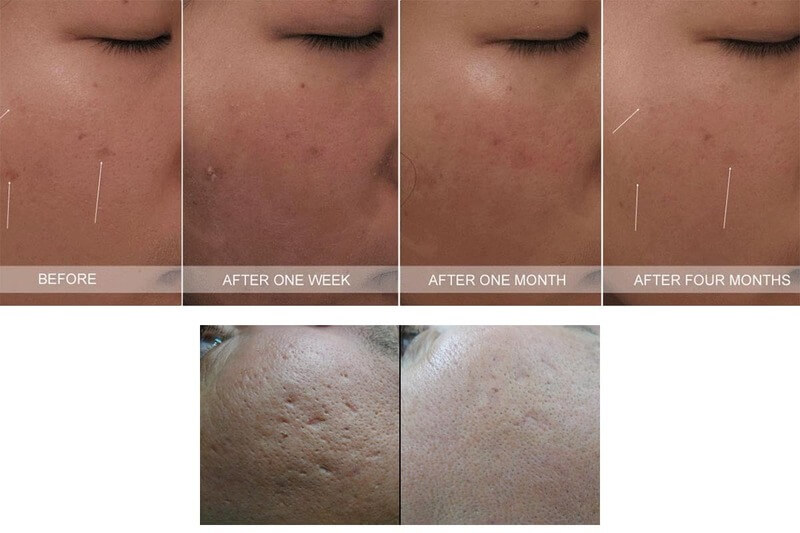
- Khunger et al. (2011): researchers examined the safety and efficacy of CROSS in dark skin types (Fitzpatrick IV and V). 30 patients were given a priming regimen of 4% hydroquinone, 0.025% tretinoin, and sunscreen for 2 weeks, before 4 sessions of 100% TCA at 2 week intervals. Excellent results were seen in 73% of patients, good results in 20%, and fair results in 6.7%. Temporary hyperpigmentation was seen in 2 patients and hypopigmentation in 1 patient but there were no significant side effects like prolonged pigmentation or scarring. (13)
- Agarwal et al. (2015): another Indian study; this one used 70% TCA CROSS on 53 patients with atrophic scars every 2 weeks for 3 months. Good or excellent results were seen in 66% of patients based on physician and patient assessments. (14)
TCA Peel: Comparison & Combination Studies
In addition to stand-alone studies on TCA, there's growing evidence that a combination approach with microneedling, subcision, and/or laser therapy yields the best results:
- Leheta et al. (2012): researchers compared the effects of Baker-Gordon phenol to percutaneous collagen induction (a.k.a. microneedling) plus 20% TCA. 24 patients with atrophic scars received either 1 session of phenol or 4 sessions of M+TCA. Significant scar improvement was seen in both groups with an average improvement of 75% in the phenol group and 69% in the M+TCA group. This makes microneedling with 20% TCA a viable alternative to deep peels with a much lower risk of complication. (20)
- Leheta et al. (2012): a related study that compared non-ablative fractional laser to microneedling plus 20% TCA. 39 patients received 6 sessions of either i) M+TCA, ii) 1,540nm fractional laser, or iii) alternating sessions of the both treatments. Scar severity scores improved by 60% in group i), 62% in group ii), and 78% in group iii), and the difference was statistically significant. This shows that a combination of laser, microneedling, and TCA can lead to better aesthetic outcomes. (21)
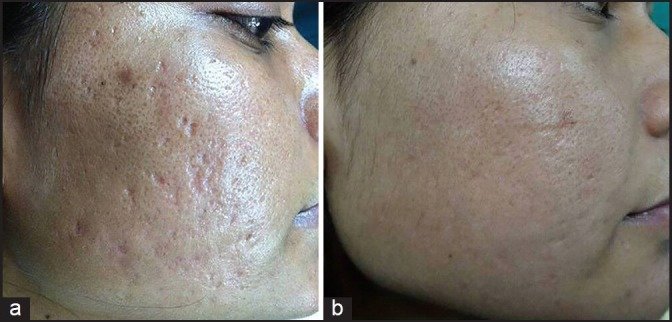
- Garg et al. (2014): an Indian study that combined subcision, microneedling, and 15% TCA to treat atrophic scars. 50 patients received 6 sessions at 2 week intervals. Scars were graded according to Goodman and Baron's qualitative scar scale. Of patients with grade 4 scars (the highest level), 37.5% improved to grade 3 scars and 62.5% to grade 2 scars. Of patients with grade 3 scars, 68% improved to grade 2 scars, 9% to grade 1 scars, and 23% to no scars at all. Overall, the treatment improved both moderate and severe scars with high patient satisfaction. (22)
- El-Domyati et al. (2017): a study of 24 patients with atrophic scars that compared microneedling alone, with platelet-rich plasma (PRP), or with 15% TCA. Patients received 6 sessions at 2 week intervals. Photographic evidence and punch biopsies showed that microneedling with PRP or 15% TCA was more effective than microneedling alone (greater epidermal thickness and better collagen remodeling). Moreover, microneedling with 15% TCA was superior to microneedling with PRP. (23)
- Taylor et al. (2017): a US retrospective study of 114 patients with mostly rolling scars who received a single combination treatment of 20% TCA, subcision, and CO2 laser. The average improvement was 2.9 (on a scale of 1-4) and 90% of patients were satisfied with their final results. This shows that TCA can be used to prepare the skin (by removing the epidermis and upper dermis) before more invasive procedures like subcision and laser therapy. (24)
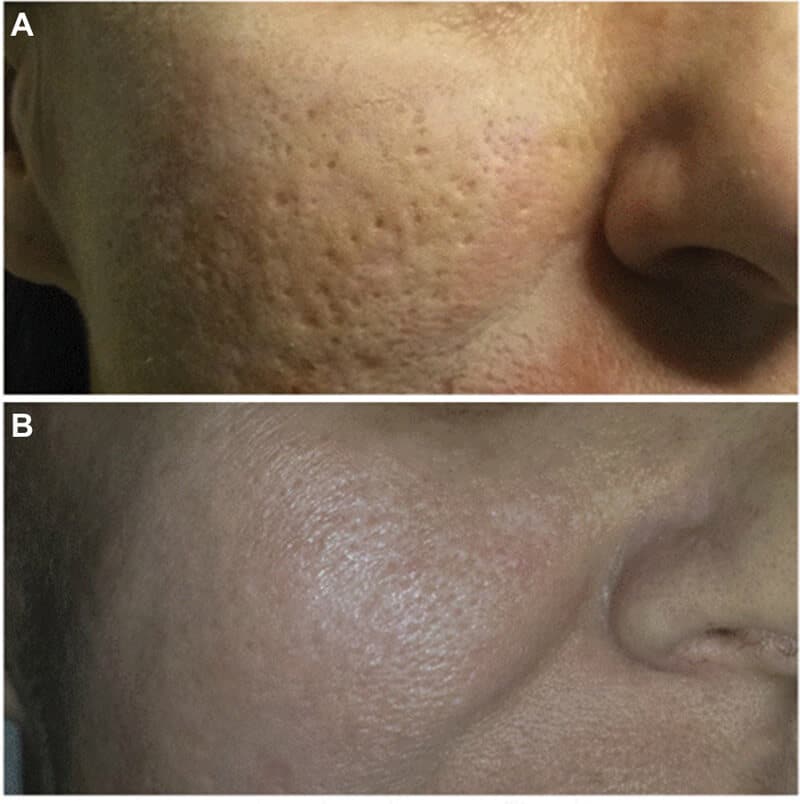
- Deprez (2019): this study presents a new technique ("anterior chemabrasion") where the skin is manually exfoliated with sandpaper before applying a topical anesthetic followed by 15% TCA. The author reports that results are as good or better than existing methods. Notably, there's a downtime of ~7 days during which a yellow scab must remain on the patient's face (bismuth subgallate powder). (25)
- Al-Hamamy (2020): an Iraqi study of 13 patients that used 25% TCA followed by separate repeated dermasanding sessions (various numbers for each patient). The authors reported statistically significant improvement in acne scar scores, especially after multiple dermasanding sessions. (26)
TCA CROSS: Comparison & Combination Studies
Similarly, TCA CROSS has been used in combination therapy:
- Kang et al. (2009): a Korean study that combined TCA CROSS (called "dot peeling"), subcision, and fractional laser. 10 patients received this combined therapy for a year (2 sessions of CROSS and subcision 2-3 months apart and laser therapy every 3-4 weeks). All patients reported improvements and acne scar severity scores decreased by ~55% on average with no significant complications. (27)
- Ramadan et al. (2011): an Egyptian study that compared 100% TCA CROSS to subcision for treating rolling scars. 20 patients received 1 to 3 sessions of CROSS on one side of their face and subcision on the other side. Researchers found that subcision produced better results with fewer side effects, but TCA CROSS produced more significant decrease in scar depth over time. (28)
- Leheta et al. (2011): another Egyptian study; this one compared 100% TCA CROSS to percutaneous collagen induction (a.k.a. microneedling). 30 patients received either 4 sessions of TCA CROSS or 4 sessions of microneedling every 4 weeks. 100% of patients experienced scar improvements with an average improvement of 75% in the TCA CROSS group and 68% in the microneedling group. The difference between the two groups was not statistically significant. (29)
- Nofal et al. (2014): this study compared PRP injections, microneedling with PRP, and 100% TCA CROSS. 45 patients with atrophic scars received 3 sessions of one of these treatments at 2 week intervals. All three groups showed statistically significant scar improvements (however, the % was not specified). (30)
- Kaur et al. (2014): researchers used subcision and 50% TCA CROSS to treat 10 patients with atrophic scars with 3 sessions at 4 week intervals. A priming regimen and post-op routine was prescribed and scars were graded using Goodman and Baron's qualitative scar scale, physician assessment, and patient questionnaire. Overall, 6 patients had excellent results, 3 had good results, and 1 had fair results. (31)
- Chae et al. (2014): a Korean study that compared 100% TCA CROSS to Phenol CROSS (which was previously not used in medical practice). 24 patients were assigned to receive either 2 sessions of TCA CROSS or 2 sessions of Phenol CROSS every 8 weeks. Scars were graded using the ECCA scale, physician assessment, and patient satisfaction. ECCA scores improved by 22% in the TCA group and 19% in the Phenol group and there was no significant statistical difference between them. (32)
- Ahmed et al. (2014): a study that compared pinpoint irradiation technique using CO2 laser against TCA CROSS. 28 patients received 4 sessions at 3 week intervals. The researchers concluded that CO2 laser was more effective than TCA CROSS based on more significant improvements in acne scar severity scores. (33)
- Dalpizzol et al. (2016): a Brazilian study that followed up Chae et al. (2014) by comparing 90% TCA CROSS to 88% Phenolic Acid CROSS. This non-randomized clinical trial included 15 patients with ice pick and boxcar scars. TCA CROSS was performed on the right side and Phenol CROSS on the left side of the face. Researchers found that both techniques produced statistically significant results (% not specified); however, 90% TCA was associated with more complications like hypochromia and enlarged scars. (34)
- Bahl et al. (2020): researchers at Boston University performed a retrospective analysis of patients who received CROSS and non-ablative fractional laser in the same session. In the study of 25 patients, the average improvement was 2.1 after 3 sessions and 2.8 after 5 sessions on a 5-point scale (0-4). All patients were satisfied (24% were very satisfied); however, one patient developed a temporary hypertrophic scar. (35)
Are There Any Side Effects Or Complications?

You should be aware of the following potential side effects and complications. (3)
Immediate
- Itching, Burning, or Irritation (caused by sensitive skin, high TCA concentration, etc.)
- Persistent Redness (caused by history of photosensitivity)
- Eye Complications (i.e. due to accidental spillage)
Delayed
- Infections (such as reactivation of herpes simplex virus due to picking the skin)
- Scarring or Poor Wound Healing
- Post-Inflammatory Hyperpigmentation (most common in darker skin types)
Prevention Tips
- Follow a priming regimen of 2-4% hydroquinone (or a product like Meladerm) for 2-4 weeks to reduce your risk of developing PIH (stop 3-5 days before the peel)
- Apply sunscreen religiously before and after the peel
- During the peel, apply a touch of Vaseline to the corners of your eyes, nose, mouth, and any particularly sensitive areas
- Always start with a lower concentration and work your way up
With proper precautions, research shows that the risk of complications can be minimized, even in darker skin types. (12, 13, 17, 26, 31, 32)
TCA Aftercare Instructions
Here's my personal post-peel aftercare routine:
- After using a chemical peel neutralizer and/or thoroughly washing with cold water, apply a sheet mask like this one by Dermal Korea (super cheap and great quality!). After a peel is the best time for your skin to soak in some extra hydration and the sheet mask helps reduce redness and irritation as well.
- In the following 5-7 days, use your regular moisturizer or cream while your skin peels and new skin cells are pushed up (this is called "re-epithelialization"). I like to use Clinique Dramatically Different Gel+ and La-Roche Posay Cicaplast Baume B5.
- Avoid sun exposure and apply adequate sunscreen during the day (SPF 30+).
- If you are concerned about hyperpigmentation, continue using a melanin inhibitor like 2-4% hydroquinone or a vitamin C serum following the peel.
Save on Pinterest:

Sources
(1) Soleymani T, et al. A Practical Approach to Chemical Peels: A Review of Fundamentals and Step-by-Step Algorithmic Protocol for Treatment. J Clin Aesthet Dermatol. 2018;11(8):21-28. PubMed
(2) Gold MH, et al. Updated International Clinical Recommendations On Scar Management: Part 2 - Algorithms For Scar Prevention And Treatment. Dermatol Surg. 2014;40(8):825-831. PubMed
(3) Anitha B. Prevention Of Complications In Chemical Peeling. J Cutan Aesthet Surg. 2010;3(3):186-188. PubMed
(4) Nikalji N, et al. Complications Of Medium Depth And Deep Chemical Peels. J Cutan Aesthet Surg. 2012;5(4):254-260. PubMed
(5) Krueger N, et al. The History Of Aesthetic Medicine And Surgery. J Drugs Dermatol. 2013;12(7):737-42. PubMed
(6) Monash, S. The Uses Of Diluted Trichloroacetic Acid In Dermatology. Urol Cutan. 1945;49;119-120. Google Scholar
(7) Gozali MV, et al. Effective Treatments Of Atrophic Acne Scars. J Clin Aesthet Dermatol. 2015;8(5):33-40. PubMed
(8) Lee JB, et al. Focal Treatment Of Acne Scars With Trichloroacetic Acid: Chemical Reconstruction Of Skin Scars Method. Dermatol Surg. 2002;28(11):1017-1021. PubMed
(9) Pastar I, et al. Epithelialization in Wound Healing: A Comprehensive Review. Adv Wound Care (New Rochelle). 2014;3(7):445-464. PubMed
(10) Yug A, et al. Histologic Study Of Depressed Acne Scars Treated With Serial High-Concentration (95%) Trichloroacetic Acid. Dermatol Surg. 2006;32(8):985-990. PubMed
(11) Fabbrocini G, et al. Cross Technique: Chemical Reconstruction Of Skin Scars Method. Dermatol Ther. 2008;21 Suppl 3:S29-S32. PubMed
(12) Bhardwaj D, et al. An Assessment of the Efficacy and Safety of CROSS Technique with 100% TCA in the Management of Ice Pick Acne Scars. J Cutan Aesthet Surg. 2010;3(2):93-96. PubMed
(13) Khunger N, et al. Evaluation Of CROSS Technique With 100% TCA In The Management Of Ice Pick Acne Scars In Darker Skin Types. J Cosmet Dermatol. 2011;10(1):51-57. PubMed
(14) Agarwal N, et al. Therapeutic Response Of 70% Trichloroacetic Acid Cross In Atrophic Acne Scars. Dermatol Surg. 2015;41(5):597-604. PubMed
(15) Nelson BR, et al. Pilot Histologic And Ultrastructural Study Of The Effects Of Medium-depth Chemical Facial Peels On Dermal Collagen In Patients With Actinically Damaged Skin. J Am Acad Dermatol. 1995;32(3):472-478. PubMed
(16) Kang, et al. The Effect Of TCA Chemical Peel On Acne Scars. Korean J Dermatol. 1996;34(6):919-923. Elsevier
(17) Al-Waiz MM, et al. Medium-depth Chemical Peels In The Treatment Of Acne Scars In Dark-skinned Individuals. Dermatol Surg. 2002;28(5):383-387. PubMed
(18) Carniol PJ, et al. Evaluation Of Acne Scar Treatment With A 1450-nm Midinfrared Laser And 30% Trichloroacetic Acid Peels. Arch Facial Plast Surg. 2005;7(4):251-255. PubMed
(19) Puri N. Efficacy of Modified Jessner's Peel and 20% TCA Versus 20% TCA Peel Alone for the Treatment of Acne Scars. J Cutan Aesthet Surg. 2015;8(1):42-45. PubMed
(20) Leheta TM, et al. Deep Peeling Using Phenol Versus Percutaneous Collagen Induction Combined With Trichloroacetic Acid 20% In Atrophic Post-acne Scars; A Randomized Controlled Trial. J Dermatolog Treat. 2014;25(2):130-136. PubMed
(21) Leheta TM, et al. Do Combined Alternating Sessions Of 1540 Nm Nonablative Fractional Laser And Percutaneous Collagen Induction With Trichloroacetic Acid 20% Show Better Results Than Each Individual Modality In The Treatment Of Atrophic Acne Scars? A Randomized Controlled Trial. J Dermatolog Treat. 2014;25(2):137-141. PubMed
(22) Garg S, et al. Combination Therapy In The Management Of Atrophic Acne Scars. J Cutan Aesthet Surg. 2014;7(1):18-23. PubMed
(23) El-Domyati M, et al. Microneedling Combined With Platelet-rich Plasma Or Trichloroacetic Acid Peeling For Management Of Acne Scarring: A Split-face Clinical And Histologic Comparison. J Cosmet Dermatol. 2018;17(1):73-83. PubMed
(24) Taylor MB, et al. Single Session Treatment of Rolling Acne Scars Using Tumescent Anesthesia, 20% Trichloracetic Acid Extensive Subcision, and Fractional CO2 Laser. Dermatol Surg. 2017;43 Suppl 1:S70-S74. PubMed
(25) Deprez P. "Anterior" Chemabrasion For Acne Scars Treatment. Clin Cosmet Investig Dermatol. 2019;12:141-149. PubMed
(26) Al-Hamamy HR, et al. Evaluation Of Treatment of Acne Scars with 25% Trichloroacetic Acid Chemical Peel Followed By Manual Dermasanding. J Cosmet Dermatol. 2020;10.1111/jocd.13754. PubMed
(27) Kang WH, et al. Atrophic Acne Scar Treatment Using Triple Combination Therapy: Dot Peeling, Subcision And Fractional Laser. J Cosmet Laser Ther. 2009;11(4):212-215. PubMed
(28) Ramadan SA, et al. Subcision Versus 100% Trichloroacetic Acid In The Treatment Of Rolling Acne Scars. Dermatol Surg. 2011;37(5):626-633. PubMed
(29) Leheta T, et al. Percutaneous Collagen Induction Versus Full-concentration Trichloroacetic Acid In The Treatment Of Atrophic Acne Scars. Dermatol Surg. 2011;37(2):207-216. PubMed
(30) Nofal E, et al. Platelet-rich Plasma Versus Cross Technique With 100% Trichloroacetic Acid Versus Combined Skin Needling And Platelet Rich Plasma In The Treatment Of Atrophic Acne Scars: A Comparative Study. Dermatol Surg. 2014;40(8):864-873. PubMed
(31) Kaur J, et al. Subcision Plus 50% Trichloroacetic Acid Chemical Reconstruction Of Skin Scars In The Management Of Atrophic Acne Scars: A Cost-effective Therapy. Indian Dermatol Online J. 2014;5(1):95-97. PubMed
(32) Chae WS, et al. A Comparative Study Of The Efficacy And Safety Of 100% TCA Cross And Phenol Cross For Atrophic Acne Scarring. Korean J Dermatol. 2014;52(5):293-301. Korean Dermatological Association
(33) Ahmed R, et al. Randomized Clinical Trial Of CO₂ Laser Pinpoint Irradiation Technique Versus Chemical Reconstruction Of Skin Scars (CROSS) In Treating Ice Pick Acne Scars. J Cosmet Laser Ther. 2014;16(1):8-13. PubMed
(34) Dalpizzol M, et al. Comparative Study of the Use of Trichloroacetic Acid and Phenolic Acid in the Treatment of Atrophic-Type Acne Scars. Dermatol Surg. 2016;42(3):377-383. PubMed
(35) Bahl A, et al. Treatment Of Atrophic Acne Scars With Combination Therapy Of Chemical Reconstruction Of Skin Scars Method And Fractionated Nonablative Laser: A Retrospective Analysis. J Cosmet Dermatol. 2020;10.1111/jocd.13514. PubMed


